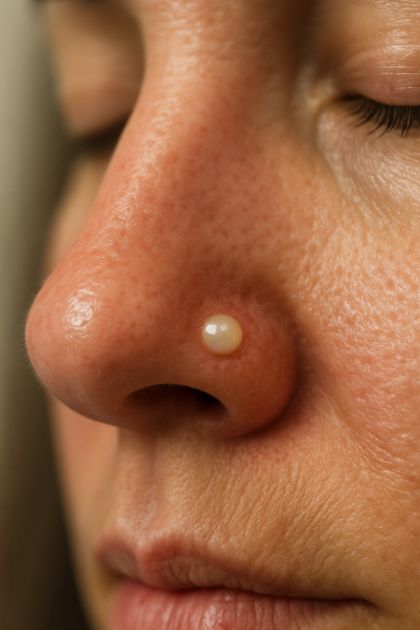
Basal cell carcinoma is a cancer type of the skin that begins in the basal cells which are located on the skin's surface, epidermis. It is mainly due to long-term exposure of ultraviolet (UV) from the sun or tanning beds. BCC is characterized by its slow growth and low likelihood of metastasis: it rarely spreads to other parts of the body. But if left without treatment, it can wreak havoc in the vicinity by infiltrating nearby tissues. Early diagnosis and remedy are crucial in stopping complications.
Risk Factors for Skin Cancer. The development of skin cancer, especially basal cell carcinoma, is influenced by a variety of risk factors. For example, having fair skin, light hair and light-colored eyes, which are particularly susceptible to UV damage. A history of frequent sunburns, especially childhood sunburns, is still another key risk factor. Additional factors to consider: age (BCC is more prevalent in older adults) Personal or family history of skin cancer. People with compromised immune systems are also at risk, and some chemicals are bad news for them, including arsenic.
The Significance of Early Detection. If diagnosed early, skin cancer can be treated more effectively and severe complication rates can frequently be minimized. For patients with established risk, it is recommended that they should undergo and annually check their skin regularly, a health care professional may perform the self-examinations. When existing moles change or new skin lesions form, timely diagnosis and treatment can also arise. Early intervention is usually of a less invasive nature and is associated with an improved chance of full recovery.
8. Emergency Action and Tools for Relief. Some temporary measures taken while awaiting a specialist appointment can relieve symptoms and work wonders for the time being. Excess topical treatments like hydrocortisone cream and other over-the-counter products will reduce inflammation and irritation. If you can still keep the area clean and moisten it, it can minimize the risk of secondary infection by using. Avoiding sun rays that damage by wearing a hat or a high-SPF sunscreen might also allow the area to grow healthier by preventing sun. But these are just ad hoc solutions that should not replace professional medical advice.
How to Watch for Changes at Home. Home monitoring has routine observation and documentation. Keep accurate photographic records of the lesion, with detailed, written photographs taken every couple of weeks to match your angles and lighting for comparison. Using a ruler, measure the bump and include any changes in size, tone or texture. Asking for any symptoms (pain, bleeding, etc.) would be helpful and it can show you some specific details so you can document your treatment to your health manager during your session.
Getting Ready for a Specialist Visit. Get all information about the bump, photographs, measurements and symptom history as necessary well in advance of the specialist's visit. Record any questions or concerns you have and address them in the consultation. And make sure your medical history — previous skin problems and family history of skin cancer — comes up before the appointment. The specialist will use this information to make an accurate diagnosis and to design an appropriate treatment plan.
Management for the Long Term and Prevention. Management of skin lesions in the long term entails periodical follow-up and anti-routine practice to avoid relapse. That encompasses everything from protective clothing and using sunscreen with elevated SPF to avoid ultraviolet exposure. Regular follow-up appointments must remain a reality for anyone with a skin cancer history. These appointments enable ongoing surveillance and early intervention upon the start of new lesions. And a simple healthy lifestyle that includes a balanced diet and non-tobacco can be beneficial for overall skin health.